

Because insulin is so closely linked to our diet, we should start there. Sugar, flour, bread, and pasta, among other highly processed carbohydrates, are known to raise blood glucose levels and insulin production. The carbohydrate hypothesis (also known as the insulin theory) has been used to justify the creation of many low-carb diets.
These beliefs aren’t new; the first low-carbohydrate diets were developed in the nineteenth century. The first of them is thought to have been written by William Banting, who introduced the first commercial weight loss diet in his brochure The 1863 “Letters on Obesity.” Banting weighed less than 92 kilogrammes and had attempted but failed to lose weight by eating less and exercising more.
After failing to lose weight, Banting followed his doctor’s advice and stopped eating bread, milk, beer, sweets, and potatoes, which had previously been an important part of his diet. Banting helped people lose weight, and a successful and healthy keto diet has been widely used to treat obesity for many years. Despite low-carb diets’ success, the insulin theory is flawed. While high consumption of processed carbohydrates plays a role in raising insulin levels, it is not the only factor.
Insulin is the key that unlocks the cell’s door to glucose entry. Normal glucose levels no longer open the door when dealing with insulin resistance, and glucose builds up in the bloodstream.
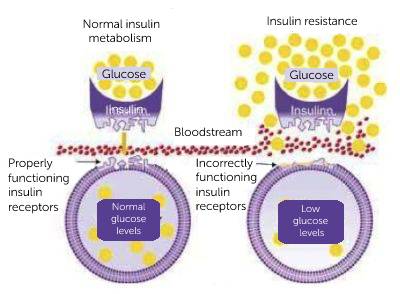
The body produces more insulin to overcome resistance and push glucose into the cell. This brings blood sugar levels back to normal, but at the cost of long-term hyperinsulinemia. Insulin resistance is critical because it leads to weight gain. What is the process of making it?
Type 2 diabetes is characterised by a high level of insulin resistance. Because obesity usually occurs 10 years before the diagnosis of type 2 diabetes, many people believe that obesity causes insulin resistance. Weight loss is frequently linked to a decrease in insulin sensitivity. Obesity causes insulin resistance, which is followed by pre-diabetes and type 2 diabetes. Obese people have significantly increased insulin resistance when compared to lean people.
It hasn’t been easy to figure out how obesity causes insulin resistance. Fatty acids in the blood were the first suspects, as their levels rise with obesity. Insulin activates the LPL by transporting it to adipocytes where it can be stored. Fatty acid levels in the blood should not be high unless insulin is not working properly. In other words, fatty acid levels rise as a result of insulin resistance, not the other way around. The fact that the release of fatty acids into the blood does not increase insulin resistance supports this theory.
What if it wasn’t the fatty acids that were to blame? Adiponectin, resistin, and interleukin 6 were all suspected, but it was impossible to prove that they were the cause of insulin resistance.
Because the hormonal cause of insulin resistance has yet to be discovered after 35 years of intensive research, it’s safe to rule out obesity as a factor. Their relationship is the subject of three theories. Obesity, for starters, can lead to insulin resistance. This, however, does not explain how lean people can develop type 2 diabetes. Insulin resistance, on the other hand, can lead to obesity. Obesity usually occurs before insulin resistance, so this is unlikely. Years of intensive research have failed to establish the validity of any of the above theories. There’s also the possibility of a third option. Obesity and insulin resistance can both be caused by metabolic syndrome, which you can learn more about on this page.
Receive tips, articles and all the goodies absolutely free, straight to your inbox!